For approximately thirty several years, the hunt for a get rid of for Alzheimer’s condition has targeted on a protein referred to as beta-amyloid. Amyloid, the hypothesis goes, builds up inside the brain to deliver about this memory-robbing disorder, which afflicts some 47 million men and women throughout the world.
Billions of bucks have poured into building therapies aimed at cutting down amyloid — consequently much, to no avail. Trials of anti-amyloid therapies have repeatedly failed to help people, sparking a reckoning among the field’s leaders.
All together, some researchers have toiled in the relative shadows, building opportunity tactics that target other areas of cells that go awry in Alzheimer’s: molecular pathways that control power generation, or clean up cellular debris, or control the move of calcium, an ion essential to nerve mobile purpose. And ever more, some of these researchers have targeted on what they suspect may well be an additional, more central factor in Alzheimer’s and other dementias: dysfunction of the immune system.
With the field’s thinking narrowed all-around the amyloid speculation, immunological suggestions have struggled to win favor — and funding. “There was no traction,” suggests Malú Tansey, a College of Florida neuroscientist whose do the job focuses on immunology of the brain. The committees that critique grant apps did not want to hear about immunological studies, she suggests.
But around the earlier 10 years, the immune system link to Alzheimer’s has become clearer. In several enormous studies that analyzed the genomes of tens of 1000’s of men and women, lots of DNA variants that have been connected to heightened Alzheimer’s risk turned out to be in genes included in immunity — particularly, a department of the body’s defenses recognized as the innate immune system. This department assaults viruses, micro organism and other invaders speedily and indiscriminately. It operates, in section, by triggering irritation.
A more link amongst irritation and Alzheimer’s turned up in March 2020, in an assessment of digital wellness data from 56 million people, such as about 1.six million with rheumatoid arthritis, psoriasis and other inflammatory disorders. When researchers searched all those data for Alzheimer’s diagnoses, they uncovered that people taking drugs that block a key molecular bring about of irritation, referred to as tumor necrosis factor (TNF), have about 50 to 70 % lessen odds of owning an Alzheimer’s diagnosis than people who have been prescribed all those drugs but did not consider them.
This more recent wave of studies opened people’s eyes to the plan that the immune system may be a important driver of Alzheimer’s pathology, suggests Sharon Cohen, a behavioral neurologist who serves as healthcare director at the Toronto Memory System in Canada. Over time, Cohen suggests, researchers began thinking that “maybe irritation is not just an aftereffect, but basically a pivotal, early outcome.”
Tansey is attempting to harness this escalating realization to establish new therapies. A drug she helped to establish approximately twenty several years ago relieved Alzheimer’s-like functions in mice and not long ago confirmed encouraging effects in a tiny review of men and women with the condition. “I consider we have been on to one thing way back when,” she suggests.
Tansey got interested in neurodegenerative condition in the late nineties, while operating as a postdoctoral fellow at Washington College in St. Louis. Her investigation targeted on molecules that boost the survival of sure neurons that degenerate in Parkinson’s condition — in lab dish experiments, in any case. But immediately after 6 several years on a meager postdoc wage, and with her spouse about to start out neurology education at UCLA, she took a career at a biotech company in the Los Angeles location, referred to as Xencor. She tackled a project that the company experienced on the back burner: designing new drugs to inhibit that inflammatory molecule TNF.
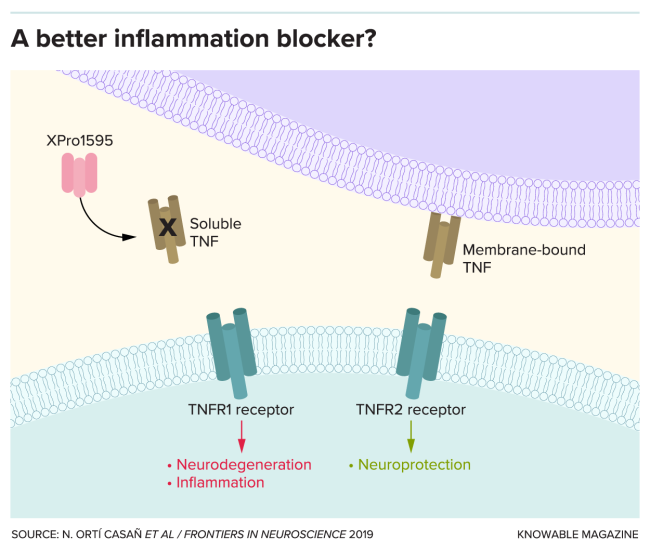
At the time, medical professionals now employed two this sort of drugs to handle autoimmune disorders this sort of as psoriasis and rheumatoid arthritis. But these drugs have hazardous side consequences, mostly owing to TNF’s difficult biology. TNF arrives in two forms: one particular that is anchored to the membranes of cells, and a soluble type that floats all-around in the spaces in amongst. The soluble TNF causes irritation and can kill cells contaminated with viruses or micro organism — it’s a essential career but, in excess, destroys healthful tissues. The membrane-sure type of TNF, on the other hand, confers protection in opposition to infection to get started with. The drugs in use at the time inhibited both of those forms of TNF, leaving men and women at risk for bacterial infections by viruses, micro organism and fungi that ordinarily only cause complications for men and women with weakened immune techniques.
Working with genetic engineering, Tansey and her Xencor colleagues intended a drug that helps prevent this likely dangerous side outcome by concentrating on only the hazardous, soluble type of TNF. It gloms on to the hazardous TNF and will take it out of circulation. In checks, injections of the drug diminished joint inflammation in rats with a affliction akin to arthritis.
By the time the do the job was published in Science in 2003, Tansey experienced returned to academia, starting up up her possess lab at the College of Texas Southwestern Clinical Middle in Dallas. And as she scoured the scientific literature on TNF, she began to consider once again about all those experiments she’d completed as a postdoc, on neurons ruined for the duration of Parkinson’s condition. She go through studies demonstrating that the brains of Parkinson’s people have high degrees of TNF — and she wondered if TNF could be killing the neurons. There was a very clear way to discover out: Put the TNF-blocking drug she’d helped to establish at Xencor into the brains of rats that have been manipulated to establish Parkinson’s-like symptoms and enjoy to see what happened.
Her hunch proved proper — the drug slowed the decline of neurons in Parkinson’s rats. And that led Tansey to wonder: Could TNF also be included in the decline of neurons in other forms of neurodegeneration, such as Alzheimer’s condition? Mulling around the nuanced roles of innate immune cells, which appear to help or damage relying on the context, she started off rethinking the prevailing amyloid speculation. Maybe, she thought, amyloid ends up clumping in the Alzheimer’s brain due to the fact immune cells that would ordinarily gobble it up get sluggish as men and women age: In other words, the amyloid accrued as a consequence of the condition, not a cause.
The double-edged nature of immune activity also meant that our immune techniques may, if unchecked, exacerbate complications. In that case, blocking areas of immune purpose — particularly, irritation — may show practical.
The plan that blocking irritation could maintain cognition and other areas of brain purpose has now uncovered help in dozens of studies, such as several by Tansey’s lab. Working with an approach that induced Alzheimer’s-like neurological symptoms in mice, neuroscientist Michael Heneka, a researcher at Germany’s College of Bonn, and his colleagues uncovered that mice engineered to absence a key molecule of the innate immune system didn’t form the hallmark amyloid clumps uncovered in Alzheimer’s.
Tansey and colleagues, for their section, confirmed that relieving irritation with the drug Tansey helped establish at Xencor, referred to as XPro1595, could reduce amyloid buildup and strengthen nerve mobile connections in mice with Alzheimer’s-like memory complications and pathology. Her crew has also uncovered that mice on a substantial-fats, substantial-sugar diet regime — which causes insulin resistance and drives up Alzheimer’s risk — have reduced inflammation and enhanced behavior on checks of sociability and nervousness when taken care of with XPro1595.
All told, hints from human genetic and epidemiologic facts, combined with escalating proof from mouse models, “was shifting or pointing towards the function of the immune system,” suggests Heneka, who coauthored a 2018 short article in the Annual Critique of Drugs about innate immunity and neurodegeneration. And the proof is escalating: In 2019, a review of more than 12,000 older grownups uncovered that men and women with persistent inflammation suffered better psychological losses over a period of time of twenty several years — a clue, once again, that irritation could be an early driver of cognitive decline.
The accumulating facts certain Tansey that it was time to test this plan in men and women — that “instead of concentrating on amyloid, we need to start out concentrating on the immune system,” she suggests. “And it requirements to be early.” Once far too substantially hurt is completed, it may well be extremely hard to reverse.
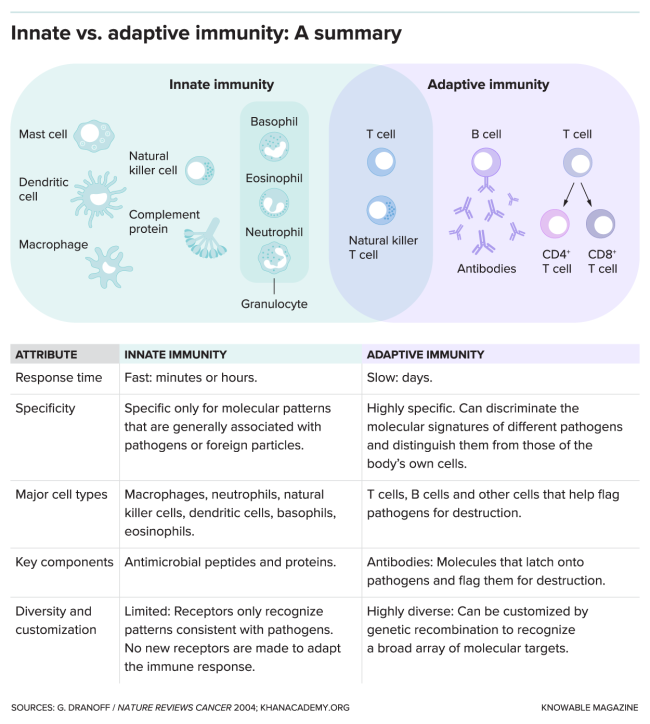
Immune-based mostly tactics in opposition to Alzheimer’s are now becoming pursued, but most are quite distinctive than what Tansey was proposing. Corporations largely do the job with the “adaptive” immune system, which assaults pathogens or molecules really particularly, recognizing them and marking them for destruction. Experimental therapies include things like antibodies that figure out amyloid and target it for removing.
INmune Bio, in La Jolla, California, is one particular of several biotech organizations taking a distinctive approach: attempting to fight degenerative brain condition by concentrating on the less unique innate immune system. “The immune system is a fifty-fifty partnership,” suggests RJ Tesi, the CEO. “If you’re about to have a prize fight, you’re not going to leap in with one particular hand tied guiding your back. Likewise, with Alzheimer’s or most cancers, you do not want to go into the ring with 50 percent the immune system becoming ignored.” To pursue this approach, INmune Bio purchased industrial legal rights to XPro1595. (Tansey is a paid consultant for INmune Bio but is not included in any of the company’s trials.)
INmune Bio initially targeted on most cancers, so when it intended its Alzheimer’s demo, it employed a approach typically employed in most cancers drug trials. In Tesi’s perspective, a key motive that experimental most cancers drugs succeed much more generally than experimental neurology drugs is the use of molecular condition indicators called biomarkers. These are actions this sort of as genetic variants or blood proteins that help to distinguish people who, from the outside, may well all appear to have the exact similar condition, but may well basically differ from one particular an additional.
By working with biomarkers to decide on individuals, most cancers researchers can enroll the people most most likely to answer to a offered drug — but lots of neurology trials enroll people based mostly only on their prognosis. And that is problematic, suggests Tesi, due to the fact researchers are coming to recognize that a prognosis of Alzheimer’s, for instance, may basically encompass a variety of subtypes of condition — each with its possess underlying biology and each, maybe, necessitating a distinctive treatment.
In an ongoing demo of XPro1595, INmune Bio aims to enroll 18 men and women with mild to reasonable Alzheimer’s condition, all of whom have elevated degrees of biomarkers for abnormal irritation, such as one particular referred to as C-reactive protein. In July, the company claimed early facts from 6 individuals who have been taken care of with the TNF inhibitor when a 7 days for 12 weeks and assessed for brain irritation working with a specialized magnetic resonance imaging (MRI) system.
Over the 12-7 days period of time, brain irritation fell 2.three % in 3 individuals who obtained the substantial-dose TNF inhibitor — compared with a 5.1 percent improve in twenty five Alzheimer’s people whose facts have been collected previously as section of a major long-phrase study of Alzheimer’s condition. Three individuals who got a small dose of XPro1595 experienced a scaled-down — 1.seven % — improve in brain irritation. In this tiny demo, the researchers did not observe variations in cognition. But their MRI assessment confirmed that inflammation was diminished by about 40 percent in a specific bundle of nerve fibers referred to as the arcuate fasciculus that is significant for language processing and small-phrase memory.
“It’s early times,” Cohen suggests — interim effects in just 6 men and women. “However, in a tiny sample dimensions like that, you may not expect to see nearly anything.” Previous studies of anti-inflammatory drugs did not clearly show a profit in Alzheimer’s people, but researchers are now reexamining these demo failures, Cohen suggests. “Maybe the plan of the immune system is significant, but our therapies have been far too blunt,” she suggests.
It’s not just INmune Bio that has researchers psyched about the prospect of tinkering with innate immunity to tackle brain condition. Alector, a South San Francisco biotech company, is building opportunity therapeutics to activate the innate immune system to fight Alzheimer’s. Some of their experimental drugs are meant to boost the activity of innate immune cells in the brain referred to as microglia. Tiaki Therapeutics in Cambridge, Massachusetts, meanwhile, is working with computational approaches to detect opportunity therapies for men and women with neuroinflammatory disorders who have unique gene signatures. And an additional company, Shanghai-based Green Valley, is investigating a drug that incorporates a combine of seaweed sugars that, the company statements, alters intestine micro organism to tamp down brain irritation.
It’s encouraging to see so lots of distinctive techniques to harnessing the innate immune system to fight Alzheimer’s, Heneka suggests. He predicts, however, that a variety of therapies will be desired to tackle this sort of a multifaceted, difficult condition.
But Tansey suspects that persistent irritation is a critical factor that will take a toll on the brain around the program of lots of several years. Though decreasing irritation will not address all the things, she suggests, “I consider it will purchase you a ton. Simply because it’s the darkish passenger of the journey.”
Just before going freelance in 2014, immunologist-turned-journalist Esther Landhuis (@elandhuis) included investigation on neurodegenerative disorders as a reporter for the information website Alzforum. This short article originally appeared in Knowable Magazine, an impartial journalistic endeavor from Annual Opinions.
